
Partial Hospitalization Program vs Intensive Outpatient Program – Comprehensive Addiction Treatment Options Explained
Choosing the right level of care between a Partial Hospitalization Program (PHP) and an Intensive Outpatient Program (IOP) starts with understanding how each option balances clinical intensity, daily structure, and real-world responsibilities. This article explains what PHP and IOP are, how they work, and how they fit into the continuum of addiction treatment so you can match clinical need with practical realities. Many people and families struggle to decide when to step down from inpatient care or when outpatient addiction treatment is adequate; the correct choice reduces relapse risk, addresses co-occurring disorders, and preserves life roles like work and family. You will learn clear definitions, sample schedules, candidate profiles, and decision factors that clinicians use, plus a practical look at transitions from detox and inpatient care into day treatment programs. The guide also covers differences in supervision and therapies, shows where PHP and IOP sit in a stepped-care pathway, and provides actionable insurance-verification steps and access tips. Throughout, terms like intensive outpatient program, partial hospitalization program, PHP treatment Las Vegas, and dual diagnosis are used to link clinical concepts to practical planning for recovery.
What is a Partial Hospitalization Program in Addiction Treatment?
A Partial Hospitalization Program (PHP) is a structured day treatment program that provides intensive clinical services without 24/7 residential stay, delivering a high level of supervision and medical oversight during daytime hours. PHP works by concentrating multiple evidence-based therapies into daily blocks so patients receive comprehensive assessment, medication management, individual and group psychotherapy, and skills training while returning home or to a sober living environment each evening. The clinical goal of PHP is stabilization and rapid skill acquisition to reduce acute symptoms and prepare patients for continued outpatient care, making PHP a common step-down from inpatient rehab or medical detox. Current research and care models emphasize PHP’s role in addressing both substance use disorders and co-occurring mental health concerns through coordinated multidisciplinary teams.
How is PHP structured and what therapies does it include?
PHP is typically scheduled as a multi-hour day program five or more days per week, combining clinical monitoring with intensive therapy and medical services. A sample PHP day often includes morning medical check-ins or medication management, several hours of group therapy focused on relapse prevention and coping skills, individual therapy slots, and family therapy or case management in the later day. Core therapy modalities in PHP commonly include cognitive behavioral therapy (CBT), dialectical behavior therapy (DBT) skills groups, motivational interviewing, and trauma-informed care approaches to address underlying drivers of substance use. Medical oversight in PHP involves psychiatric evaluation, medication-assisted treatment as appropriate, and regular clinical review to guide step-down readiness and ensure safety.
- This list outlines common PHP therapy components and structure:Morning medical and medication management checks, ensuring physiological stabilization and medication adherence.Several hours of group therapy each day focused on relapse prevention, coping skills, and psychoeducation.Individual therapy and family sessions scheduled to address personal and relational factors that affect recovery.
These elements create an intensive, coordinated day treatment environment that supports stabilization while preserving community ties and independent living. Understanding PHP’s structure leads naturally to identifying who benefits most from this level of care and what measurable advantages it provides.
Who are the ideal candidates for PHP and what are its benefits?
Ideal PHP candidates are adults with moderate to severe substance use disorders who require structured daily care but do not need 24-hour inpatient medical monitoring, including those stepping down from inpatient rehab or completing medical detox. Clinical indicators for PHP include recent relapse with elevated risk, incomplete stabilization after detox, significant psychiatric symptoms that need close follow-up, or a living situation that supports evening safety and sobriety. Primary benefits of PHP include rapid access to intensive therapeutic hours, ongoing medication management, collaborative case management, and accelerated skill-building that reduces hospital readmission and supports transition to lower-intensity outpatient care. For individuals whose lives include work, family responsibilities, or housing stability, PHP provides a therapeutically rich alternative that balances clinical intensity with community reintegration.
What is an Intensive Outpatient Program and How Does it Work?
An Intensive Outpatient Program (IOP) is an outpatient addiction treatment level that delivers structured therapy and support several times per week while allowing participants to maintain most daily responsibilities such as work or school. IOP works by concentrating therapy sessions—commonly totaling 9–15 hours per week—into evening or daytime blocks, combining group therapy, individual counseling, and relapse prevention skills training with flexible scheduling. The core value of IOP is its balance: people receive clinically meaningful treatment sufficient for many mild-to-moderate cases or as a step-down after PHP, but with less medical supervision than PHP. For many patients, IOP supports sustained recovery through community-based supports and ongoing case planning while minimizing disruption to employment and family life.
What is the typical structure and therapy approach in IOP?

A typical IOP schedule includes multiple weekly sessions—often 3–5 days a week—with each session lasting two to four hours and a mix of group process, skills training, and individual check-ins. Therapy modalities in IOP frequently feature cognitive behavioral therapy for relapse prevention, motivational enhancement to sustain change, group-based process work to build peer support, and practical life-skills modules addressing triggers and coping. Many programs offer flexible options such as evening groups or telehealth check-ins to accommodate work or school, and case management supports to coordinate community resources and medication management when needed. This combination allows patients to practice recovery skills in their day-to-day environment while receiving structured clinical feedback and peer accountability.
- IOP commonly emphasizes these therapy components and scheduling features:Group therapy focused on relapse prevention and skills practiced in real life settings.Individual counseling sessions to set personalized goals and monitor progress.Flexible scheduling options, including evening groups or telehealth, to support work and family commitments.
These structural features make IOP particularly suited to people who have stable housing, lower medical acuity, and supportive community environments. The practical flexibility of IOP naturally leads to considering who benefits most and how these advantages compare with higher-intensity day treatment options.
Who benefits most from IOP and what are its key advantages?
IOP benefits individuals with mild-to-moderate substance use disorders, stable medical and psychiatric status, and strong social supports who need structured therapy without residential care. Advantages of IOP include greater scheduling flexibility, lower cost compared with day hospital-level care, easier integration with work or school obligations, and strong emphasis on community-based relapse prevention resources. Because IOP participants remain in their daily environments, they can immediately apply coping skills to real-world triggers while receiving structured therapeutic feedback and peer support. IOP also functions well as a step-down from PHP or inpatient treatment, helping to maintain gains made during more intensive care while gradually reducing clinical contact.
What are the Key Differences Between PHP and IOP?
PHP and IOP differ primarily in intensity, hours of clinical contact, level of medical and psychiatric oversight, and setting; these differences determine suitability for individual patients and clinical outcomes. PHP typically provides more intensive daily hours, closer medical supervision, and a primary focus on stabilization and transition planning, while IOP emphasizes flexibility, fewer weekly hours, and community-based practice of recovery skills. Choosing between them depends on measurable criteria such as recent medical instability, psychiatric symptoms, housing safety, and the need for medication-assisted treatments. Clinicians use these dimensions—intensity, supervision, time commitment, and setting—to recommend the most appropriate step in the continuum of care.
- Intensity: PHP provides day-long therapeutic blocks; IOP offers several shorter sessions weekly.
- Time commitment: PHP often runs 20+ hours/week; IOP usually runs 9–15 hours/week.
- Supervision: PHP includes daily medical and nursing oversight; IOP has less frequent clinical checks.
- Setting: PHP is clinic-based day treatment; IOP is outpatient with community integration.
| Program Level | Attribute | Typical Value |
|---|---|---|
| Partial Hospitalization Program (PHP) | Weekly hours and schedule | 20+ hours per week; daily attendance, clinic-based day treatment |
| Intensive Outpatient Program (IOP) | Weekly hours and schedule | 9–15 hours per week; multiple sessions across days, often evenings |
| PHP vs IOP | Clinical oversight | PHP: daily medical/psychiatric monitoring; IOP: regular but less frequent clinical review |
How do intensity, time commitment, and supervision differ between PHP and IOP?
Intensity, time commitment, and supervision are the central clinical variables guiding placement decisions: PHP delivers more concentrated therapeutic hours with daily medical oversight, while IOP offers fewer weekly hours and less intensive medical monitoring. Quantitatively, PHP typically operates as a day treatment program with multiple hours daily and frequent medication management checks, appropriate for those needing close symptom stabilization. IOP commonly provides evening or daytime sessions totaling under 15 hours weekly, emphasizing skills practice and community reintegration for those with lower clinical acuity. Safety considerations such as recent detox, suicidal ideation, or uncontrolled psychiatric symptoms usually prompt recommendation for PHP rather than IOP.
What distinguishes PHP and IOP in terms of setting, focus, and patient suitability?
Setting differences—clinic day treatment for PHP versus community-based outpatient sessions for IOP—shape the therapeutic focus and candidate suitability; PHP’s setting supports stabilization and medical interventions, while IOP’s setting emphasizes maintenance and application of recovery skills. PHP is often selected for patients with higher clinical needs, those transitioning from inpatient care, or those whose living environments require added daytime structure. IOP is better suited for patients with stable housing, lower medical risk, and sufficient social supports who can practice recovery strategies in real-world contexts. Examples include a patient stepping down from inpatient rehab to PHP for a few weeks, then moving into an IOP as symptoms stabilize and community supports strengthen.
Where Do PHP and IOP Fit in the Continuum of Addiction Care?
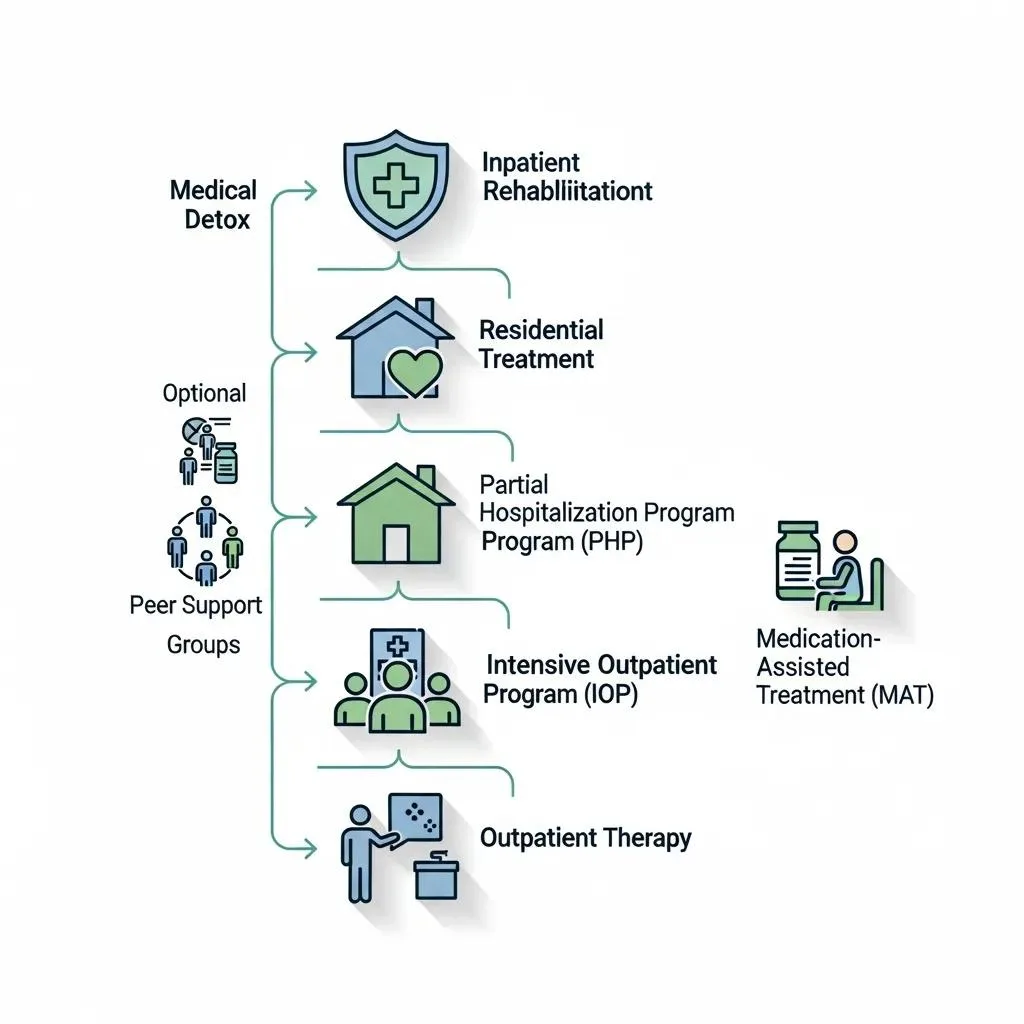
PHP and IOP occupy middle-to-lower intensity tiers in the addiction care continuum, providing critical transitional care between inpatient/medical detox and standard outpatient therapy. The typical sequence progresses from medical detox for acute withdrawal management to inpatient rehab when 24/7 care is required, then to PHP as a day treatment step-down for stabilization and intensive therapy, followed by IOP for skills consolidation, and finally to regular outpatient therapy and community-based aftercare. Each level serves a distinct role: detox addresses immediate physiological risk, inpatient manages high clinical acuity, PHP accelerates stabilization with therapeutic hours, and IOP sustains recovery in daily life. This graduated pathway allows clinicians to match intensity to risk and recovery milestones.
| Level of Care | Attribute | Typical Sequence / Role |
|---|---|---|
| Medical Detox | Purpose | Manage acute withdrawal and physiological stabilization; often first step |
| Inpatient Rehab | Purpose | 24/7 residential care for high-acuity stabilization and intensive therapy |
| Partial Hospitalization Program (PHP) | Role | Step-down day treatment to continue intensive therapy while returning home each night |
| Intensive Outpatient Program (IOP) | Role | Lower-intensity outpatient treatment to practice and maintain recovery skills |
| Standard Outpatient | Role | Ongoing counseling and community supports for long-term relapse prevention |
How do PHP and IOP relate to medical detox and inpatient rehab?
PHP and IOP typically follow medical detox and inpatient rehab when initial physiological and high-acuity psychiatric needs have been managed; detox addresses withdrawal, and inpatient care addresses severe instability or safety concerns. After detox, if a patient shows persistent psychiatric symptoms or needs structured daytime support, clinicians commonly recommend PHP as the next step to continue medication management and intensive therapy. When patients demonstrate stability, reduced cravings, and improved coping skills under PHP, the clinical team may recommend transitioning to IOP to promote community-based skill application. These transition triggers—stabilization of withdrawal symptoms, reduced suicidal ideation, and consistent engagement in therapy—are standard decision points in contemporary care models.
What is the role of PHP and IOP in ongoing recovery and relapse prevention?
PHP and IOP both deliver relapse prevention curricula, skill-building modules, and case management that form the foundation for long-term recovery planning and aftercare linkage. Typical relapse prevention components include identifying triggers, developing coping strategies, engaging peer supports, and establishing sober routines and contingency planning. Aftercare planning in PHP and IOP focuses on referrals to community groups, outpatient therapists, vocational supports, and ongoing medication management when indicated. Peer support and community resources are emphasized so patients can transition from structured clinical settings into sustainable, community-based recovery networks that reduce relapse risk.
How Does BetterChoice Treatment Center Deliver PHP and IOP Services in Las Vegas?
BetterChoice Treatment Center provides a continuum of addiction services in Las Vegas that includes medical detox and inpatient rehab alongside PHP and IOP options, enabling coordinated step-down care when indicated. The center emphasizes personalized treatment plans delivered by a multidisciplinary team in a comfortable, upscale setting, combining clinical rigor with comfort to support engagement and retention in care. BetterChoice accepts major insurance providers and holds recognized accreditations that reflect quality standards; these include Nevada’s Health Workforce acknowledgments, LegitScript approval, and the Joint Commission Gold Seal of Approval. Continuity of care is supported by 24/7 assistance and family support services, facilitating smooth transitions from acute care into PHP and then into IOP or outpatient follow-up.
What makes BetterChoice’s PHP and IOP programs unique and effective?
BetterChoice’s PHP and IOP programs are framed around evidence-based therapies delivered via a multidisciplinary team, personalized treatment planning, and a facility environment designed to reduce barriers to engagement. The program model pairs clinical behavioral therapies with structured case management and medication management when clinically necessary, aiming to address both substance use and co-occurring psychiatric conditions in an integrated way. Accreditation by respected organizations and acceptance of major insurance providers support trust and access for families seeking verified standards of care. Taken together, these elements create a coordinated pathway that emphasizes safety, individualized treatment goals, and sustained recovery planning.
How does BetterChoice support co-occurring disorders within PHP and IOP?
BetterChoice approaches co-occurring disorders through integrated assessment and concurrent treatment, ensuring psychiatric evaluation and medication management are coordinated alongside addiction-focused therapies. Clinical teams at the center assess mental health needs early, apply evidence-based interventions such as CBT and trauma-informed care, and coordinate psychiatry input when medication-assisted treatment or psychotropic medications are indicated. Care coordination includes case management and family support to address social determinants that affect mental health and substance use outcomes. This integrated model helps reduce fragmentation of care and supports simultaneous stabilization of both substance use and mental health symptoms.
What Should You Know About Insurance Coverage and Access for PHP and IOP?
Understanding insurance coverage and access is essential for timely placement into PHP or IOP, as pre-authorization, benefit verification, and documentation can affect program start dates and out-of-pocket costs. BetterChoice accepts major insurance providers and encourages verification of specific benefits before admission; patients and families should prepare policy numbers, subscriber details, and recent clinical notes when initiating a benefits check. Key insurance considerations include medical necessity criteria, prior authorization requirements, co-pay and deductible responsibilities, and documentation of recent clinical encounters such as detox or inpatient discharge summaries. Proactive verification and coordinated case management can streamline access to day treatment programs and reduce administrative delays in starting clinically indicated PHP or IOP services.
| Consideration | Attribute | Patient Action / Tip |
|---|---|---|
| Pre-authorization | Requirement varies by insurer | Collect policy info and request benefits check early to determine coverage for PHP/IOP |
| Medical necessity | Clinical documentation needed | Obtain recent detox or inpatient discharge notes to support level-of-care requests |
| Cost sharing | Co-payments and deductibles apply | Ask insurer about out-of-pocket estimates and prepare documentation for appeals if needed |
Which insurance providers does BetterChoice accept for PHP and IOP?
BetterChoice accepts major insurance providers, which facilitates access for many patients seeking PHP or IOP services in Las Vegas; however, coverage details and pre-authorization rules vary by plan and medical necessity determinations. Patients should gather their insurance card information, subscriber details, and any recent clinical documentation such as detox records or psychiatric assessments before contacting the provider for verification. A benefits check confirms covered services, prior authorization needs, and estimated patient financial responsibility, and it also helps identify required diagnosis codes or clinical summaries. Verifying these items early reduces uncertainty and supports faster initiation of the appropriate day treatment program.
- Steps to verify insurance coverage with a treatment provider:Collect insurer name, policy number, subscriber information, and employer details from your insurance card.Request a benefits check from the treatment provider, specifying PHP or IOP services and asking about pre-authorization requirements.Obtain and save any authorization codes, denial letters, or appeal instructions you receive from the insurer.
How can patients and families navigate insurance and payment options?
Navigating insurance and payment options involves a stepwise approach: gather documentation, request a benefits check, follow up on pre-authorization, and prepare for potential appeals or alternative arrangements if coverage is limited. Begin by compiling policy details, recent clinical notes, and any provider recommendations that document medical necessity; then ask the provider to submit a benefits verification and, if needed, a pre-authorization request. If coverage is partial or denied, consider working with the center’s case management to explore appeals, sliding-scale resources, or referrals to community programs that align with clinical needs. Maintaining clear communication with both insurer and treatment team reduces delays and keeps focus on clinical stability and recovery.
- Practical checklist for insurance navigation:Gather policy card, subscriber details, and recent clinical documentation.Request a benefits check and ask about pre-authorization requirements.Keep written records of authorization numbers, appeal instructions, and contact names.
