
Medications for Opioid Detox: A Clear, Compassionate Guide to Safe Withdrawal and Recovery
Opioid detox is a medically supervised process that helps the body clear opioids while minimizing danger and discomfort. Medications are a core part of that care: they stabilize brain chemistry, ease withdrawal symptoms, lower cravings, and reduce the risk of complications. This guide walks you through the medications commonly used in opioid detox, how they work, what withdrawal often feels like and when it peaks, and practical expectations for patients and families considering medication-supported detox. Trying to quit alone can lead to severe symptoms and make recovery much harder — evidence-based medications make withdrawal safer, more tolerable, and more likely to lead into ongoing treatment. You’ll read about primary options like buprenorphine/naloxone (Suboxone), naltrexone (including injectable Vivitrol), methadone programs, and non‑opioid supports such as clonidine and lofexidine. We also explain how Medication-Assisted Treatment (MAT) pairs medications with counseling, what intake and daily care normally look like, insurance basics, and how families can help while respecting privacy. Continue for practical timelines, side-by-side comparisons, and clear next steps for people in Nevada seeking safe, respectful care.
What Is Opioid Detoxification and Why Are Medications Essential?
Opioid detoxification is the medical process that manages the physical and emotional withdrawal that follows stopping opioid use. Medications are essential because they calm overactive receptors, reduce sympathetic symptoms (like rapid heart rate and sweating), and lower the chance of relapse. By targeting opioid receptors or easing autonomic symptoms, medications shorten the worst parts of withdrawal, help prevent dehydration and other complications, and make it possible for patients to engage in therapy and follow-up care. Medical detox is different from quitting alone: it combines vital-sign monitoring, tailored medications, and supportive care to treat both body and mind. Below is a quick summary of the main benefits of medication-supported detox and why supervised care improves safety and outcomes.
Medication-supported detox offers several immediate clinical advantages:
- Better control of vomiting, diarrhea, and dehydration through symptom management.
- Reduced craving intensity, which helps patients participate in counseling and planning.
- Safer tapering or stabilization on long-acting medications to lower overdose risk.
These practical benefits make medication-assisted detox appropriate for many people with opioid use disorder and guide decisions about which medications best match a person’s history and recovery goals.
How Does Medical Detox Support Opioid Withdrawal?
Medical detox combines targeted medications with continuous clinical monitoring to reduce symptom severity and catch complications early. Clinicians check vitals, adjust medication doses, and treat problems such as severe agitation, dehydration, or cardiac issues to keep patients safe. Nursing staff perform regular assessments, give medications on schedule, and coordinate with prescribing clinicians as withdrawal progresses. This structured care prevents avoidable emergencies and creates a stable window to begin longer-term treatment like maintenance medications or relapse-prevention strategies.
Those safety measures also allow behavioral therapies and discharge planning to start while patients are stabilized — preparing them for the next steps in recovery and clarifying typical symptom timelines.
What Are Common Opioid Withdrawal Symptoms and Their Timeline?
Opioid withdrawal usually follows a predictable pattern rooted in receptor changes. Early signs appear within hours, symptoms often peak in a few days, and most acute physical symptoms ease within one to two weeks — although some discomfort or mood changes can last longer. For short-acting opioids, early symptoms typically begin 6–24 hours after the last dose; long-acting opioids may take longer to show. Early signs include yawning, runny nose, anxiety, and muscle aches. Peak withdrawal (24–72 hours) can add nausea, vomiting, diarrhea, intense cravings, and sleep problems. By about one week many physical symptoms have declined, though mood swings, low mood, and cue-triggered cravings may persist. Understanding this timeline helps clinicians decide when to start certain medications (for example, safe timing for buprenorphine) and helps families set realistic expectations for the course of care.
Which Medications Are Used for Opioid Withdrawal and Detox?
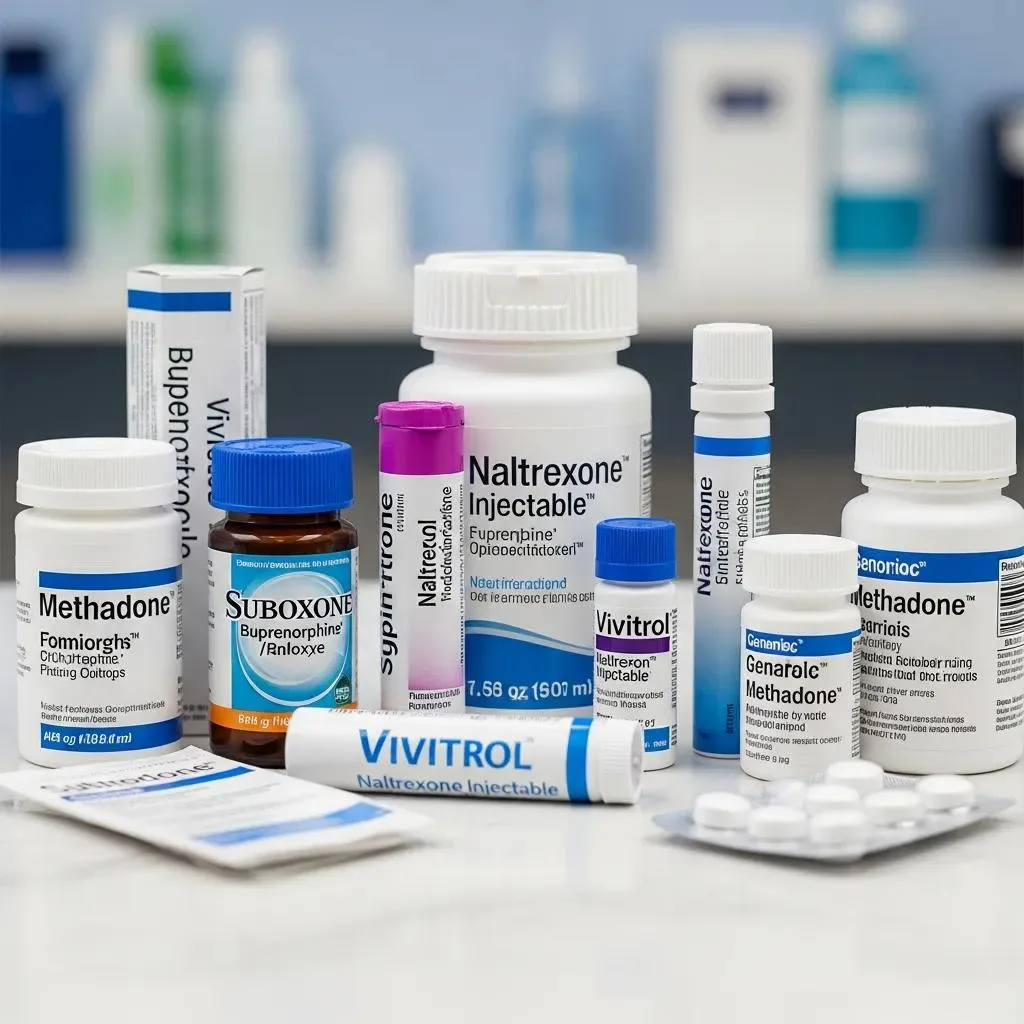
The main medications used in opioid detox include buprenorphine/naloxone (Suboxone), naltrexone (oral and injectable Vivitrol), and methadone programs. Each works through different receptor actions and is chosen based on where the patient is in withdrawal and their long-term goals. Buprenorphine is a partial opioid agonist that reduces cravings and withdrawal while carrying a ceiling effect that lowers the risk of respiratory depression; it’s commonly used to stabilize patients and transition them to outpatient care. Naltrexone is an opioid antagonist started after a full detox to block opioid effects and help prevent relapse; the injectable form (Vivitrol) offers monthly protection for patients who are opioid-free. Methadone, a full agonist provided through regulated clinics, can be used for detox or long-term maintenance with daily supervision. The table below summarizes these options for quick reference.
| Medication | Mechanism | Typical Timing in Care | Main Benefits |
|---|---|---|---|
| Buprenorphine/naloxone (Suboxone) | Partial opioid agonist; naloxone deters misuse | Usually started during mild–moderate withdrawal when clinically appropriate | Reduces cravings and withdrawal symptoms; safer respiratory profile than full agonists |
| Naltrexone (oral or injectable Vivitrol) | Opioid antagonist | Initiated after a confirmed opioid‑free period | Blocks opioid effects; supports relapse prevention without opioid exposure |
| Methadone | Full opioid agonist | Provided through regulated clinics for detox or maintenance | Effective stabilization and long‑term maintenance under supervised care |
Mechanism and timing determine each medication’s role. Choosing the right option depends on clinical assessment, prior treatment history, and the patient’s goals. The sections below describe Suboxone and naltrexone in more detail to clarify when each may be appropriate.
How Does Suboxone Aid Opioid Withdrawal?
Suboxone (buprenorphine/naloxone) eases withdrawal by partially activating mu opioid receptors—enough to reduce cravings and withdrawal but with a lower risk of full respiratory depression. Buprenorphine occupies receptors to blunt symptoms and bring stability, while the naloxone component discourages injection misuse. Clinicians generally start Suboxone when a patient is in mild to moderate withdrawal to avoid precipitated withdrawal; doses and monitoring are individualized to balance symptom relief and safety. Common side effects include constipation, headache, and mild sleepiness. Patients are watched for clinical response and potential drug interactions as part of a broader treatment plan.
Knowing how Suboxone works helps explain why antagonist approaches like naltrexone are used later in recovery planning.
What Role Does Naltrexone Play in Opioid Addiction Treatment?
Naltrexone is an opioid antagonist that blocks opioid effects and reduces the reinforcing reward of opioid use. It works best when started after a confirmed opioid‑free period to avoid precipitating withdrawal. Naltrexone comes as a daily oral pill or a monthly injectable (Vivitrol). It’s a non‑opioid option for people who have completed detox and want pharmacologic relapse prevention. Benefits include removing opioid-induced euphoria and offering a maintenance choice without ongoing opioid exposure. Limitations include the need to be opioid‑free before starting and monitoring liver function and adherence. For many patients, naltrexone is a helpful relapse‑prevention tool when combined with counseling and structured supports.
What Are Other Supportive Medications for Managing Withdrawal Symptoms?
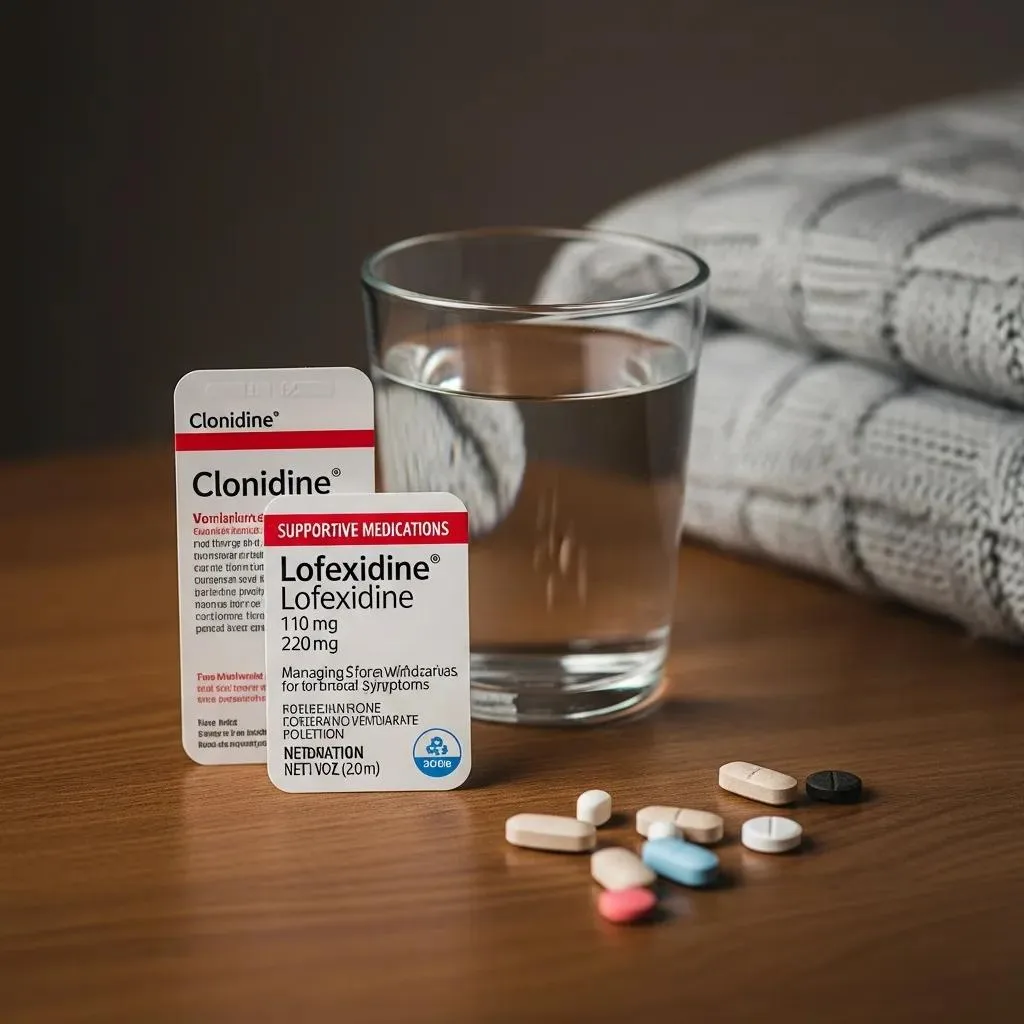
Non‑opioid supportive medications treat the autonomic and symptomatic parts of withdrawal — easing anxiety, sweating, nausea, and sleep problems — so patients can tolerate detox and engage in therapy. Clonidine and lofexidine reduce sympathetic overactivity (lowering heart rate and blood pressure); antiemetics treat nausea; antidiarrheals address loose stools; and short‑term sleep aids or antidepressants may help with insomnia or mood symptoms. Choosing supportive meds requires thinking about contraindications (for example, hypotension risk with clonidine/lofexidine) and interactions with primary detox drugs. The brief table below summarizes common supportive options, routes, and monitoring points to guide safe use during detox.
| Medication | Symptom Targeted | Route | Monitoring / Precautions |
|---|---|---|---|
| Clonidine | Autonomic symptoms (sweating, fast heart rate, anxiety) | Oral | Monitor blood pressure for hypotension; adjust dose carefully |
| Lofexidine (Lucemyra) | Sympathetic overactivity and anxiety | Oral | Watch for sedation and low blood pressure; useful when clonidine isn’t suitable |
| Symptomatic meds (antiemetics, antidiarrheals) | Nausea, vomiting, diarrhea | Oral / PRN | Track effectiveness and possible interactions with core medications |
This targeted approach lets clinicians focus on the symptoms that cause the most distress while keeping the overall plan safe and comfortable. The next sections cover methadone programs and practical use of clonidine and lofexidine in more detail.
How Do Methadone Programs Assist in Detoxification and Maintenance?
Methadone is a long‑acting full opioid agonist used in regulated clinic programs to stabilize patients, reduce illicit opioid use, and support longer‑term maintenance when appropriate. Its steady receptor activity prevents withdrawal and cravings, but because methadone is a full agonist it’s provided under strict program rules: daily dispensing in many clinics, frequent clinical assessments, and gradual dose adjustments with close monitoring for side effects. Methadone programs include routine urine testing, counseling, education about overdose prevention, and case coordination — a structure that can benefit patients who need closer supervision or who did not respond well to partial agonists. Strong program oversight helps prevent diversion and ensures safe induction and maintenance.
With that framework in place, clinicians can also use non‑opioid options like clonidine or lofexidine to manage autonomic symptoms when appropriate.
How Are Clonidine and Lofexidine Used to Alleviate Physical Withdrawal Symptoms?
Clonidine and lofexidine work on alpha‑2 adrenergic receptors to reduce norepinephrine release and calm sympathetic overactivity. They often bring symptom relief within hours, easing sweating, fast heart rate, and anxiety. Because both drugs can lower blood pressure and cause drowsiness, clinicians monitor vitals and tailor dosing to each patient. These medications are commonly used alongside antiemetics or antidiarrheals and fit into a medication‑supported detox plan as adjuncts to primary agents or as alternatives when opioid‑based medications aren’t appropriate.
How Does Medication-Assisted Treatment Integrate Medications into Recovery?
Medication-Assisted Treatment (MAT) combines medications with counseling, behavioral therapies, and support services to treat opioid use disorder as a chronic medical condition. Medications stabilize brain chemistry while psychosocial services address behaviors, triggers, and life stressors. MAT is evidence‑based: it lowers overdose deaths, improves treatment retention, and supports functional recovery when paired with therapy. Integration means choosing the right medication, ongoing medical monitoring, coordination between prescribers and counselors, and connections to social supports like housing or job resources. Typical services in a comprehensive MAT model include:
- Medication management: Regular medical review and dose adjustments to keep patients stable and safe.
- Counseling and behavioral therapies: Individual and group work to build coping skills and relapse‑prevention strategies.
- Case management and social support: Help with housing, employment, and community resources that support long‑term recovery.
These coordinated elements create a clear path from medical stabilization to ongoing recovery planning. The next section shows how we deliver this locally at BetterChoice.
What Is the Comprehensive MAT Approach at BetterChoice Treatment Center?
At BetterChoice Treatment Center we offer a local MAT model that pairs personalized medication plans with a multidisciplinary team of physicians, therapists, and nurses for continuous clinical oversight and care coordination. Our approach is rooted in compassion and evidence: 24/7 clinical support, optional holistic therapies, and individualized stabilization followed by counseling and discharge planning to reduce relapse risk. Patients move through intake, medical stabilization, ongoing counseling, and coordinated aftercare referrals — all delivered with attention to comfort and confidentiality. Accreditation and verification from LegitScript and The Joint Commission support our quality standards, and our integrated medical and psychosocial services help patients transition from detox into sustainable recovery pathways.
This program description leads into how counseling and behavioral therapies work alongside medications to improve outcomes.
How Do Counseling and Behavioral Therapies Support Medication Use?
Counseling and behavioral therapies strengthen the effects of medication by addressing thought patterns, building coping skills, and teaching relapse‑prevention techniques that drugs alone cannot provide. Evidence‑based approaches like cognitive behavioral therapy (CBT), motivational interviewing, and group therapy reduce relapse risk by helping patients manage cravings, triggers, and stress. Clinicians coordinate therapy times with medication reviews so psychosocial work aligns with pharmacologic stabilization. Together, medication plus therapy improves retention, reduces illicit use, and supports a gradual return to daily life.
What Should Patients Expect During Medication-Supported Opioid Detox?
When you enter medication‑supported detox, expect a structured intake, regular medical assessments, daily medication administration as needed, and discharge planning that connects you to outpatient services. Medications are adjusted to manage withdrawal while therapy and case management start early. Typical daily routines include medication dosing, brief medical checks, therapy sessions, rest, and symptom monitoring to keep care safe and comfortable. The table below outlines standard intake steps, who’s involved, expected timing, and what to bring to speed your entry into care.
| Step | Who Is Involved | Expected Timing | What to Bring / Prepare |
|---|---|---|---|
| 1. Initial phone/screening | Intake coordinator / clinician | Before arrival or day 0 | Photo ID, insurance card if available, list of medications |
| 2. Medical and psychiatric assessment | Physician / NP and nurse | First hours on site | Medication history and recent substance use details |
| 3. Medication initiation / stabilization | Prescribing clinician and nurse | Within the first 24 hours as indicated | Comfort items and any prior treatment records |
| 4. Therapy planning and discharge coordination | Counselor / case manager | During stay, before discharge | Contact info for aftercare and a family plan if applicable |
This operational outline reduces uncertainty and helps families plan. The following paragraphs describe daily schedules and how family contact and privacy are handled during care.
What Is the Intake Process and Daily Schedule at BetterChoice?
At BetterChoice intake begins with a thorough medical and psychiatric assessment so clinicians can choose safe, effective medications and identify any other needs. From there we create an individualized stabilization plan. Daily schedules typically include medication administration, brief medical checks, scheduled therapy or group sessions, optional holistic therapies, and rest or recovery time. We emphasize patient comfort, confidentiality, and coordinated family contact when appropriate; nursing staff and therapists are available to answer questions while protecting private health information. Knowing this routine helps patients and families prepare for the detox period.
With intake and daily routines explained, the next important practical topic is insurance coverage for these medications.
How Does Insurance Coverage Work for Opioid Detox Medications?
Insurance coverage usually starts with a benefits verification and sometimes requires prior authorization or clinical documentation to show medical necessity. Patients should bring ID and insurance information to intake. Many centers accept insurers such as Magellan Health, TRICARE, Aetna, Anthem, Blue Cross Blue Shield, Beacon Health Options, Cigna, and EmblemHealth, which can cover inpatient detox, medications, and follow‑up services depending on the plan. If coverage is limited, programs often offer financial counseling or referrals to alternative resources to avoid interruptions in care. The checklist below shows what to prepare and next steps for verification.
Checklist for insurance verification and preparation:
- Bring photo ID and your insurance card.
- Prepare a current list of medications and recent treatment history.
- Ask the intake coordinator about prior authorization timelines and coverage limits.
These steps help speed access to medication‑supported detox and reduce administrative delays during a critical window for treatment.
How Can Families Support Loved Ones Through Medication-Based Opioid Detox?
Families can support recovery by offering practical help, attending approved family education sessions, and coordinating logistics while respecting the patient’s privacy and treatment boundaries. Useful actions include arranging transportation, gathering medical records, learning about withdrawal timelines and medication roles, and joining family counseling when the patient agrees. Clear, nonjudgmental communication helps family members express concern without pushing the patient away, and understanding confidentiality rules eases anxiety about what staff can share. The list below highlights specific ways families can help while preserving autonomy and privacy.
- Prepare documentation: Collect medical history and medication lists to bring to intake.
- Provide logistic help: Arrange transportation, housing transitions, or child care during treatment.
- Seek education: Attend family sessions or request materials to better understand MAT and relapse prevention.
These supportive steps work best when coordinated with treatment staff. The following sections explain safety, privacy, and family resource options in more detail.
What Are Common Family Concerns About Safety and Privacy?
Families often worry about confidentiality, medication diversion, and overdose risk. Clinicians address these concerns by explaining privacy rules, safety protocols, and what can and cannot be shared without the patient’s consent. Under privacy protections, staff can confirm that someone is receiving services but generally cannot disclose clinical details without authorization; however, clinicians can offer general safety guidance and warning signs that need immediate attention. Treatment teams use secure medication handling, monitor for diversion, and provide naloxone education where appropriate. Giving families conversation prompts and clear guidance on when to raise safety concerns helps lower anxiety and supports helpful involvement.
With those privacy safeguards in mind, families may ask what resources BetterChoice offers to help.
What Resources and Guidance Does BetterChoice Provide for Families?
BetterChoice Treatment Center offers family-focused resources such as educational sessions, referrals to family counseling, guidance on protecting patient privacy, and help connecting to community support groups while maintaining confidentiality. Staff can advise on how to reach out in ways that respect the patient’s treatment plan, provide materials about medications and withdrawal timelines, and suggest structured next steps for family involvement. Families are encouraged to request information through intake and to join authorized family programs that improve communication and relapse‑prevention skills. These resources are designed to empower families to support recovery in positive, sustainable ways.
Frequently Asked Questions
What is the difference between detoxification and rehabilitation in opioid treatment?
Detoxification is the first stage of care focused on safely managing physical withdrawal as the body clears opioids. It usually lasts days to a few weeks and may include medications to ease symptoms. Rehabilitation refers to the longer process of addressing the psychological and behavioral aspects of addiction through therapy, counseling, and ongoing supports to prevent relapse. Both stages are important parts of a complete recovery plan.
How long does the opioid detoxification process typically take?
Detox timelines vary with the type of opioid, length of use, and individual health. Acute withdrawal often peaks within 24 to 72 hours and may last a few days to two weeks. Some people experience protracted symptoms — such as mood changes or low energy — that can linger for weeks. A clinician can give a more personalized estimate based on medical history.
Are there any risks associated with medication-assisted detox?
Medication-assisted detox is generally safer than stopping suddenly, but risks remain. Side effects of medications like buprenorphine or methadone can include sedation or breathing changes if dosed improperly. There is also potential for misuse or diversion. Continuous medical supervision reduces these risks by monitoring response, adjusting doses, and addressing side effects promptly.
Can I undergo opioid detox at home?
Home detox is not recommended for most people because severe withdrawal and complications can occur. Medical detox provides a controlled setting with professional supervision to manage symptoms, prevent dehydration, and reduce overdose risk. If you’re considering home options, discuss them with a clinician first — supervised care is safer and more effective for many people.
What role do family members play during the detox process?
Family members can provide emotional support, help with logistics, and join educational or counseling sessions if the patient consents. They can gather medical records, arrange transportation, and learn about withdrawal and medications to better support their loved one. Open, nonjudgmental communication and participation in family programs can strengthen recovery support.
What should I do if I experience a relapse after detox?
If relapse happens, seek help right away. Contact your healthcare provider or treatment program to discuss re‑engagement options. Relapse can be part of recovery for many people and offers information about triggers and treatment needs. Returning to structured care — whether through detox, MAT, or rehabilitation — can help regain stability and support long‑term recovery.
Conclusion
Medically supervised opioid detox, supported by evidence‑based medications, makes withdrawal safer and more manageable and creates a clear path into ongoing recovery. Knowing the roles of medications like buprenorphine, naltrexone, and supportive therapies helps patients and families make informed choices during this critical time. Choosing supervised care increases the chance of a safe transition into longer‑term treatment. If you’re ready to take the next step, explore our resources and contact us for compassionate, expert support.
