
Marijuana Addiction: Signs, Effects, and Practical Treatment Paths to Recovery
Marijuana addiction — clinically called cannabis use disorder (CUD) — happens when cannabis use begins to disrupt daily life, health, or relationships. If you or someone close to you is wondering whether a habit has become a problem, this guide lays out clear signs to watch for, common short- and long-term effects, and practical treatment options that help people regain control. Research shows that repeated, heavy THC exposure can lead to tolerance, withdrawal, and changes in mood or thinking. Evidence-based care ranges from medically supervised detox to residential rehab and outpatient counseling. Here, we explain how to spot CUD, what withdrawal usually looks like, which therapies work best (like CBT and MET), and how structured programs support recovery with integrated mental-health treatment. We also cover next steps for admissions, what to expect from detox and rehab, and how family involvement and insurance can help people in Nevada. Terms like THC, cannabinoids, marijuana detox, and marijuana rehab are used so you have clear, practical language for each issue.
What Are the Common Signs and Symptoms of Marijuana Addiction?

Cannabis use disorder shows up as repeated use despite negative consequences, loss of control, tolerance, and withdrawal. Repeated THC exposure changes reward pathways and coping habits, which can create cravings and poor decision-making that keep use going. Spotting these signs early improves the chance of effective help and prevents longer-term harm to work, school, or relationships. Below is a quick checklist you can use as a simple self‑assessment or share with someone you’re worried about.
Common signs and symptoms of marijuana addiction include:
- Continued cannabis use even when it causes problems at work, school, or home.
- Needing more cannabis over time to get the same effect (tolerance).
- Withdrawal when you stop: irritability, sleep issues, or reduced appetite.
- Repeated unsuccessful attempts to cut down or control use.
- Strong cravings or spending a lot of time getting or thinking about cannabis.
- Skipping social, work, or recreational activities because of use.
- Using cannabis in risky situations or as a way to cope with difficult feelings.
These items reflect DSM‑5 criteria and help distinguish casual use from clinically significant dependence. If several apply and they’re interfering with daily life, a professional assessment is a good next step to plan care and learn more about the physical and social effects of continued use.
How to Recognize Cannabis Use Disorder Symptoms
Cannabis use disorder usually develops over time and is defined by patterns, not a single event. You’ll see reduced ability to stop, more time spent using or recovering, and continued use despite relationship, work, or legal problems. Concrete examples include missing deadlines after late‑night use, preferring cannabis over family activities, or driving while impaired. A short self‑check can help: Do you use more than you intended? Have you tried and failed to stop? Has your use caused problems at home, work, or school?
Noticing these behavioral patterns helps point to likely physical signs and informs expectations for withdrawal and treatment planning.
What Behavioral and Physical Signs Indicate Marijuana Dependence?
Behavioral and physical signs often appear together when cannabis use is causing harm. Physical clues include growing tolerance (needing stronger or more THC), trouble sleeping, appetite or weight changes, slower reaction times, and difficulty concentrating. Behavioral signs include pulling away from friends or responsibilities, hiding use, spending more money on cannabis, or using it to self‑medicate anxiety or low mood. Many people also have co‑occurring issues like depression, anxiety, or other substance use, which can complicate recovery if they aren’t treated too.
Tracking both kinds of signs helps clinicians decide the right level of care: medical support for withdrawal and medication needs, and therapy to build coping skills and prevent relapse.
What Are the Short-Term and Long-Term Effects of Marijuana Use?
Short‑term effects are driven by THC acting on CB1 receptors in the brain’s endocannabinoid system, changing memory, coordination, perception, and mood. These immediate effects can impair driving and judgment, reduce short‑term memory, and in some people trigger anxiety or brief psychotic symptoms. Physically, THC can raise heart rate and, when smoked, irritate the lungs. Below we summarize short‑term impacts and compare them with longer‑term risks tied to heavy or early use.
Short-term effects of marijuana use:
- Cognitive and perceptual changes: short‑term memory lapses and altered sense of time.
- Psychomotor slowing: reduced coordination and reaction time that affect driving.
- Emotional effects: anxiety, paranoia, or sudden mood shifts in some users.
Summary: These short‑term effects increase safety risks and lower performance, so it’s best to avoid driving or operating machinery while impaired.
Long-term effects of frequent, heavy cannabis use are more gradual. They can include a higher chance of developing cannabis use disorder, persistent attention and learning difficulties (especially if use began in adolescence), ongoing motivational or mood changes for some people, and respiratory problems when cannabis is smoked. Heavy use can also worsen or bring out psychiatric symptoms in people with a predisposition to conditions like depression, anxiety, or psychosis. Biologically, long-term THC exposure changes synaptic plasticity and reward processing, which makes stopping harder and raises relapse risk.
These distinctions guide treatment: address immediate safety and withdrawal first, then follow with psychosocial rehabilitation to rebuild cognitive skills, routines, and roles.
How Does THC Impact the Brain and Body in the Short Term?
THC activates CB1 receptors and alters neurotransmitter signaling, which affects memory encoding, attention, coordination, and reward. That explains common short‑term experiences: forgetting details, slower thinking, and reduced motor control, especially with high‑potency products. Physically, THC can increase heart rate and irritate airways if inhaled; it can also provoke anxiety or paranoia in people who are susceptible. Typical short‑term examples are missing parts of a conversation, delayed reaction while driving, or sudden unease in social settings.
Knowing these mechanisms clarifies why short‑term impairment is usually reversible and why supervised detox may be recommended when withdrawal or co‑occurring issues need monitoring.
What Are the Lasting Consequences of Prolonged Cannabis Use?
Long-term heavy use can lead to ongoing functional changes for some people, such as persistent difficulties with attention and executive function—especially when use starts in adolescence. Other long‑term outcomes may include chronic bronchitic symptoms for smokers, lasting changes in motivation or mood, and an increased likelihood of cannabis use disorder that harms work or relationships. People with a family history of psychosis or preexisting mood disorders face higher risks of adverse psychiatric outcomes with heavy use.
These possible lasting effects highlight the value of early intervention and treatments that address both substance use and co‑occurring mental‑health conditions to prevent cumulative decline and support recovery.
How Is Marijuana Withdrawal Experienced and Managed?
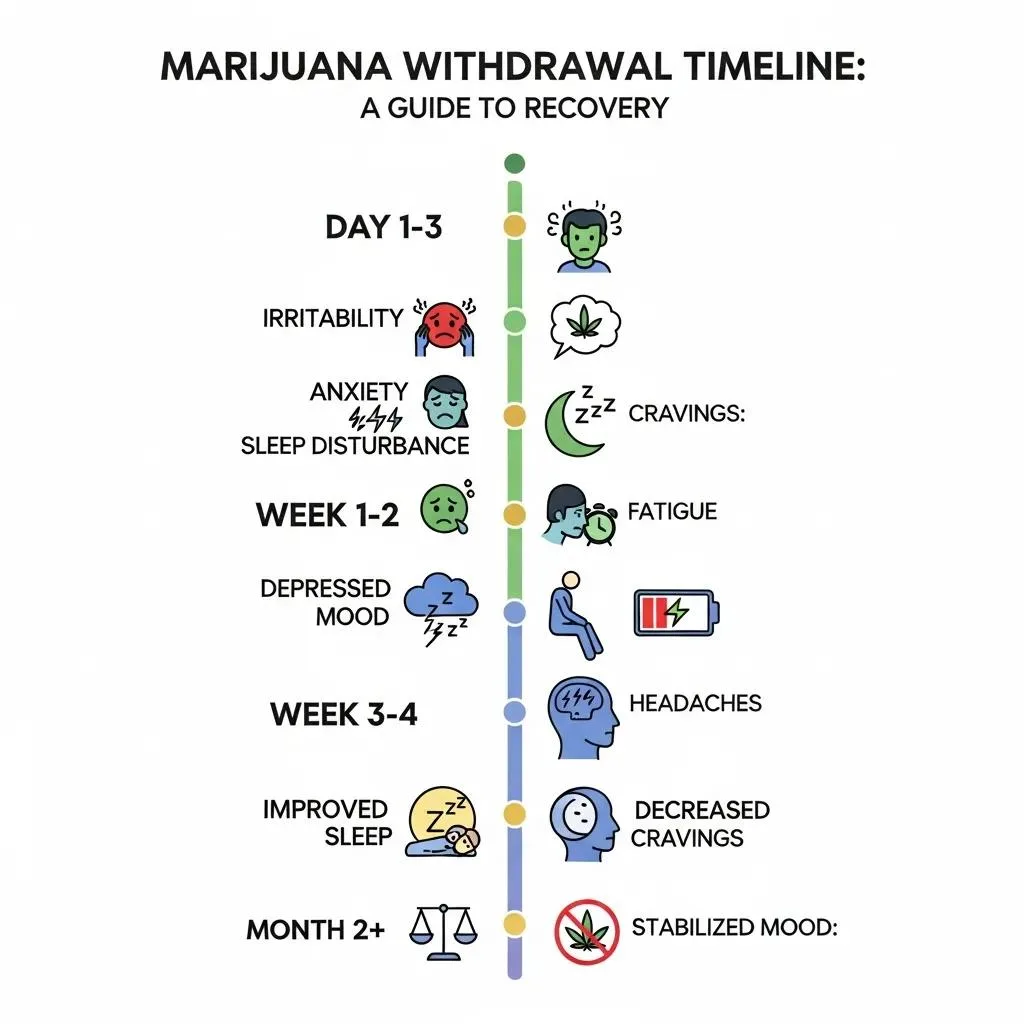
Withdrawal from marijuana typically produces a predictable set of symptoms that start within days after stopping and usually peak in the first week, with many symptoms improving over 2–3 weeks. Withdrawal reflects the brain adjusting to reduced cannabinoid signaling after repeated THC exposure and often includes mood, sleep, appetite, and physical changes. Management ranges from practical self‑care to medically supervised detox that offers round‑the‑clock monitoring, symptom‑targeted medications when appropriate, and coordination with therapy to lower relapse risk. The table below gives a quick timeline with expected severity and suggested supports.
Below is a withdrawal timeline for common symptoms and recommended supportive measures.
| Symptom Category | Typical Onset & Peak | Expected Severity & Supportive Care |
|---|---|---|
| Irritability / mood changes | Onset: 1–3 days; Peak: days 3–7 | Moderate; behavioral coping strategies, short‑term anxiolytics if clinically appropriate, counseling |
| Sleep disturbance / vivid dreams | Onset: 1–3 days; Peak: days 3–10 | Moderate; sleep hygiene, melatonin or short‑term sleep aids when indicated |
| Cravings | Onset: 1–3 days; Peak: days 2–7 | Variable; CBT techniques, motivational support, relapse‑prevention planning |
| Appetite changes / weight loss | Onset: 1–3 days; Resolution: 2–3 weeks | Mild; nutritional support and meal planning |
| Physical symptoms (headache, sweating) | Onset: 24–72 hours; Peak: days 2–5 | Mild–moderate; hydration, symptomatic care, monitoring as needed |
Summary: Most symptoms peak during the first week and ease over 2–3 weeks. Targeted supportive care makes withdrawal safer and more tolerable and lowers the chance of relapse.
What Are Typical Marijuana Withdrawal Symptoms and Their Timeline?
Common marijuana withdrawal symptoms include irritability, anxiety, sleep problems, reduced appetite, restlessness, and cravings. They usually begin within 24–72 hours after stopping and peak between days two and seven. Severity depends on how much and how long someone used, individual biology, and co‑occurring conditions. For many people, symptoms improve substantially by two to three weeks, though sleep and mood disturbances can linger for longer in some cases. Practical management focuses on regular sleep routines, hydration and nutrition, behavioral coping skills, and counseling support for cravings.
Knowing this timeline helps set realistic expectations and shows when medical detox or clinical oversight might be helpful if symptoms are severe or co‑occurring conditions exist.
How Does Medical Detox Support Safe Withdrawal from Cannabis?
Medical detox gives clinical monitoring, nursing care, and symptom‑targeted interventions that increase safety and comfort compared with quitting alone. Detox typically includes regular clinical assessments, short‑term medications for severe anxiety or sleep problems when indicated, and transition planning into ongoing therapy to address the behaviors that sustain use. This oversight reduces acute risk—especially for people with mental‑health conditions or repeated relapses—and prepares patients for the next step in rehabilitation.
The main goals during detox are stabilization and engagement. Once withdrawal is managed, patients are better able to benefit from evidence‑based therapies like CBT and MET that tackle triggers and coping strategies.
What Treatment Options Are Available for Cannabis Use Disorder at BetterChoice?
Treatment for cannabis use disorder ranges from outpatient counseling and medication‑supported strategies to structured medical detox and residential rehab. Each level of care fits different needs and levels of severity. Outpatient programs emphasize psychotherapy (CBT, MET), relapse prevention, and case management while letting patients stay at home. Inpatient rehab provides a 24/7 structured setting with group and individual therapy for people with more severe dependence or unstable living situations. Medical detox targets safe withdrawal and medical stabilization before stepping down to outpatient care. The table below compares typical length, structure, and what to expect from each level of care.
| Level of Care | Typical Length & Structure | What to Expect / Support Provided |
|---|---|---|
| Medical Detox | Short term (days to 1–2 weeks) | 24/7 clinical monitoring, symptom management, nursing support, transition planning |
| Inpatient Rehab | 2–6+ weeks structured program | Daily evidence‑based therapy, group sessions, family work, relapse‑prevention planning |
| Outpatient Programs | Weeks to months with scheduled sessions | Individual and group therapy, CBT/MET, flexible scheduling, continuing care |
| Counseling / Therapy | Variable (weekly sessions) | Targeted CBT/MET, contingency planning, treatment for co‑occurring disorders |
Summary: Matching treatment intensity to need improves safety and recovery odds by combining medical stabilization with behavioral therapies.
How BetterChoice delivers care locally: BetterChoice Treatment Center in Las Vegas offers medical detox and inpatient rehab programs designed for cannabis dependence. Our multidisciplinary teams include physicians, therapists, and nurses who create individualized treatment plans, treat co‑occurring mental‑health issues, and combine evidence‑based and holistic therapies. We provide 24/7 clinical support during higher‑acuity phases and coordinate transitions from detox to outpatient or community supports so gains made in residential care are maintained.
This local detail outlines what patients and families can expect when they choose a structured program and how accredited, multidisciplinary care supports safety and continuity.
How Does Medical Detox Facilitate Marijuana Addiction Recovery?
Medical detox helps recovery by stabilizing withdrawal symptoms, providing continuous clinical observation, and starting early therapeutic engagement to reduce relapse risk. The detox process typically includes an intake assessment, regular nursing checks, symptom management for sleep or anxiety, and psychoeducation to prepare patients for follow‑up therapy. The immediate aim is safe symptom control and a clear plan for the next level of care—whether inpatient rehab or outpatient therapy—while starting motivational work. Detox creates a foundation for CBT and MET, which target the thoughts and motivations that keep cannabis use going.
Because detox focuses on safety and immediate relief, it’s the gateway to sustained behavioral change through structured rehab services.
What Does Inpatient Rehab for Marijuana Addiction Involve?
Inpatient rehab combines structured daily programming with individual therapy, group sessions, skill‑building workshops, and holistic supports to address the psychological and behavioral causes of use. Typical days include therapy blocks (CBT, MET), relapse‑prevention education, practical coping practice, and recovery activities like mindfulness or exercise. Family sessions and discharge planning are key to building a strong aftercare plan. Length of stay varies with clinical need. The goal is to replace substance‑use routines with recovery routines, strengthen coping skills, and prepare a clear continuing‑care strategy to lower relapse risk after discharge.
This focused environment lets people do concentrated therapeutic work and practice new skills before stepping down to outpatient support.
Which Therapeutic Approaches Support Effective Marijuana Addiction Treatment?
Evidence shows behavioral therapies are the foundation of effective care for cannabis use disorder—especially cognitive behavioral therapy (CBT) and motivational enhancement therapy (MET)—often paired with contingency management and holistic supports. CBT builds coping skills and addresses unhelpful thoughts that trigger use. MET helps resolve ambivalence and build motivation for change. Contingency management rewards measurable progress in some programs, and complementary therapies like mindfulness, exercise, and nutrition support overall wellbeing and reduce relapse risk. Below is a summary of commonly used, evidence‑based approaches.
Core therapeutic approaches for cannabis recovery include:
- Cognitive Behavioral Therapy (CBT): practical skills and thought‑restructuring to reduce use.
- Motivational Enhancement Therapy (MET): short, client‑centered work to strengthen motivation and treatment engagement.
- Contingency Management: positive reinforcement for abstinence or treatment participation in some programs.
- Family Therapy and Education: works on family dynamics and builds a supportive recovery environment.
Summary: Using these therapies together addresses the psychological drivers of use and builds the behavioral skills needed for long‑term recovery. Integrated care is the standard of care.
How Do Cognitive Behavioral Therapy and Motivational Enhancement Therapy Help?
CBT helps people identify risky situations and automatic thoughts that lead to use, and it teaches practical skills—problem‑solving, activity scheduling, and urge surfing—to change behavior. MET is a brief, person‑centered approach that resolves ambivalence, sets realistic goals, and supports motivation. CBT sessions involve skill practice and homework; MET focuses on strengthening commitment and creating a doable change plan. Used together, they reduce cravings, improve coping with triggers, and increase engagement and long‑term abstinence.
Combining skill building (CBT) with motivation work (MET) gives a balanced approach that supports immediate change and long‑term recovery planning.
What Holistic Therapies Complement Cannabis Addiction Recovery?
Holistic approaches—mindfulness, yoga, exercise, nutrition counseling, and similar supports—help by improving stress management, sleep, and overall physical health, which lowers relapse vulnerability. Evidence is growing for practices like mindfulness and exercise; they can reduce craving and improve mood and attention. Practical integration usually means brief daily mindfulness practice, regular physical activity, and nutritional support to reset sleep and appetite patterns. Frequency often follows therapy schedules: daily short practices, weekly holistic sessions, and ongoing lifestyle coaching.
These therapies don’t replace evidence‑based behavioral treatments but strengthen resilience and quality of life during and after formal care.
How Can Families and Insurance Support the Recovery Journey?
Families are often the first to notice problems and can be vital in encouraging assessment and supporting recovery. Family involvement improves engagement and outcomes: offering structure, helping with logistics (appointments, transportation), joining family therapy, and learning how to support without enabling. On the insurance side, verify benefits, ask about coverage for detox and inpatient rehab, and check prior‑authorization rules to access the right care. The table below links common resources to practical action steps for families ready to take next steps.
| Resource / Coverage Type | What It Covers / Role | Action Steps / Contact Points |
|---|---|---|
| Private insurance | May cover detox, inpatient, outpatient services | Call your insurer, confirm behavioral‑health benefits, request prior authorization if required |
| Family therapy resources | Education and support to repair relationships | Schedule sessions and ask the provider for family‑inclusive care planning |
| Facility insurance verification | Confirms benefits and estimates financial responsibility | Share insurer details with the facility team so they can verify coverage and help with next steps |
| Community support groups | Ongoing peer support after discharge | Identify local or online meetings and include them in the discharge plan |
Summary: Active family involvement plus early insurance verification smooth the path to quality care and help build lasting aftercare supports.
What Resources Are Available for Family Support in Marijuana Addiction?
Families can get help through family therapy, educational workshops, and referral networks that teach communication skills, boundary‑setting, and relapse‑prevention techniques. Family sessions typically cover the effects of substance use on relationships, confidentiality limits, and practical steps to support recovery while keeping everyone safe. Peer‑led support groups and clinician‑led education sessions complement clinical work by offering shared experience and coping strategies. Bringing families into treatment early and setting clear expectations reduces caregiver stress and strengthens the patient’s support network during and after care.
Practical family involvement naturally leads to sorting out insurance and admissions steps that make beginning treatment easier.
How Does Insurance Coverage Work for Marijuana Addiction Treatment in Nevada?
Insurance coverage follows standard behavioral‑health rules: check whether detox, inpatient rehab, outpatient therapy, and specific providers are covered and whether prior authorization is required. Be ready to provide diagnosis codes and the recommended level of care; common documents include a clinical assessment, treatment plan, and provider billing details. The facility’s insurance verification team can call your insurer, explain costs, and advise on authorization timelines. Nevada residents should confirm in‑network status and ask about state mental‑health parity rules to better estimate out‑of‑pocket costs and access.
A simple verification checklist:
- Have your insurance card and subscriber information ready.
- Call your insurer to confirm behavioral‑health and substance‑use benefits.
- Ask about prior authorization rules and out‑of‑pocket limits.
- Give insurer details to the treatment facility so they can assist with verification.
Summary: Early verification and using the provider’s insurance support team reduce delays and clarify financial expectations so treatment can start sooner.
Frequently Asked Questions
What are the risks of using marijuana for individuals with a history of mental health issues?
People with anxiety, depression, or a family history of psychosis may face higher risks with marijuana use. THC can worsen mood or anxiety symptoms and, in some cases, trigger psychotic episodes in vulnerable people. If you have a mental‑health history, talk with a clinician before using cannabis—doing so can prevent complications and help protect recovery progress.
How can I support a loved one going through marijuana addiction recovery?
Support means offering a calm, nonjudgmental presence, listening, and helping them find treatment. Encourage professional help, assist with logistics like appointments and transportation, and consider family therapy to rebuild trust. Set clear boundaries to avoid enabling and balance support with expectations that promote recovery.
What role does nutrition play in marijuana addiction recovery?
Good nutrition helps restore physical health and stabilize mood and energy, which can ease withdrawal and improve cognitive function. Regular meals with whole foods—fruits, vegetables, lean proteins, and whole grains—support recovery by improving sleep, appetite regulation, and resilience against cravings.
Are there any legal implications of marijuana use in Nevada?
In Nevada, adults 21 and over can legally use marijuana for medical and recreational purposes, but rules remain: public consumption, driving under the influence, and possession limits are regulated. Federal law still classifies marijuana as illegal, which can affect employment and housing. Be aware of local rules and how use may impact legal and practical matters during recovery.
What are the benefits of group therapy in marijuana addiction treatment?
Group therapy creates a peer community that reduces isolation, builds accountability, and shares coping strategies. Hearing others’ stories and practicing social skills in a safe group setting can strengthen motivation and provide new tools for staying sober after treatment.
How can mindfulness practices aid in recovery from marijuana addiction?
Mindfulness—breathing exercises, meditation, and body awareness—helps people notice cravings or triggers without reacting. This improves emotional regulation, reduces stress, and builds the skill of pausing before acting, which is extremely helpful during withdrawal and early recovery.
Conclusion
Recognizing marijuana addiction and understanding its effects are important first steps toward recovery. Addressing both the physical and psychological sides of cannabis use disorder with evidence‑based care improves the chance of lasting change. If you or a loved one is struggling, reach out to a professional for personalized guidance. Explore our resources and take the first step toward a healthier, more stable life — you don’t have to do it alone.
